Finding a workable heart healthy diet for congestive heart failure can feel scary at first. Food is personal. We grew up with certain flavors, family recipes, holiday dishes, and comfort foods. When a cardiologist suddenly says “you need to change your diet,” it may sound like they are asking us to give up a part of our life. The good news is that a smart, realistic eating plan can protect the heart, reduce symptoms like shortness of breath and swelling, and still leave room for foods we enjoy.
What congestive heart failure does to the body
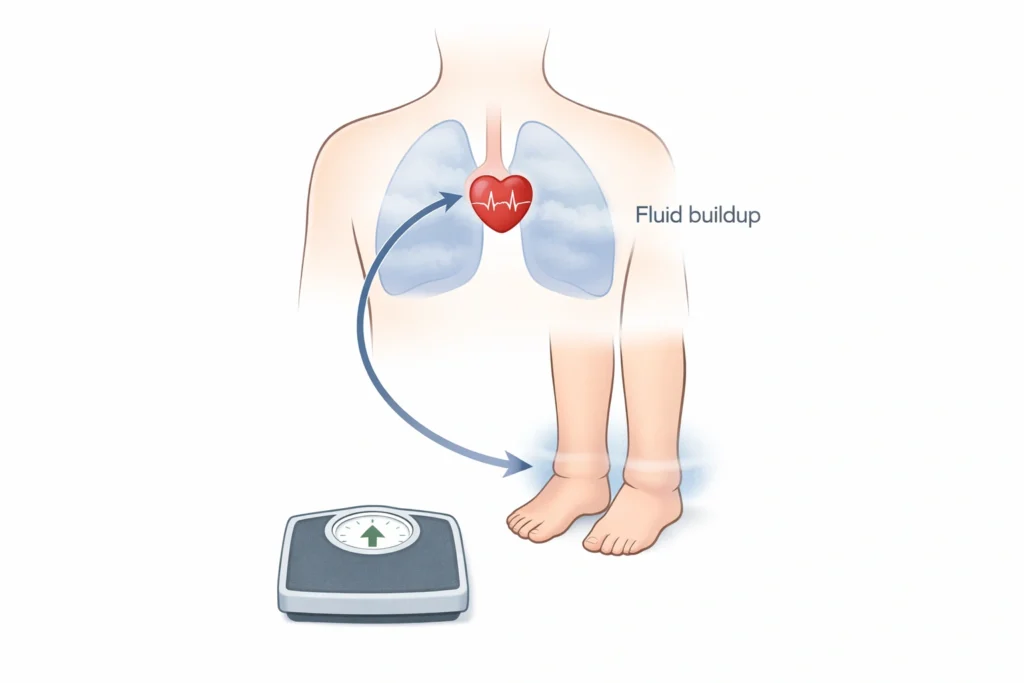
Congestive heart failure (CHF) does not mean the heart has stopped. It means the heart is not pumping blood as strong as it should. That weaker pump has a few key effects that tie directly to nutrition and daily food choices:
First, fluid builds up. When the heart can not keep up, fluid backs up into the lungs, legs, and belly. This leads to swelling, weight gain from water, waking up at night short of breath, and feeling tired just walking across the room. Second, the kidneys respond to this lower blood flow by holding on to salt and water. This is the body trying to protect blood pressure. But in CHF it usually backfires and creates even more fluid overload.
We also see changes in muscle and metabolism. Many people with moderate or severe heart failure loose muscle mass and feel weak. They may lose their appetite or get full very fast. Over time this can lead to poor nutrition, lower immune function and slower recovery from flare ups. A good heart healthy diet for congestive heart failure has to deal with all of these at once: fluid balance, blood pressure, energy intake, and long term heart protection.
Core goals of a heart healthy diet for congestive heart failure
Most cardiology and dietetic guidelines, including the American Heart Association (AHA) and American College of Cardiology (ACC), agree on four main goals for food choices when living with CHF:
- Control sodium and fluid so the body holds less water
- Support blood pressure, cholestrol and blood sugar
- Provide enough protein, vitamins, and minerals to protect muscles and organs
- Maintain a stable, healthy body weight over time
When we put those goals together, we get a pattern that looks very close to the DASH or Mediterranean eating style: lots of vegetables and fruits, whole grains, lean proteins, plant based fats, and almost no ultra processed salty foods. From experiance, patients who treat this as a flexible pattern, not a rigid “diet,” do much better in the long run.
Why sodium matters so much in heart failure
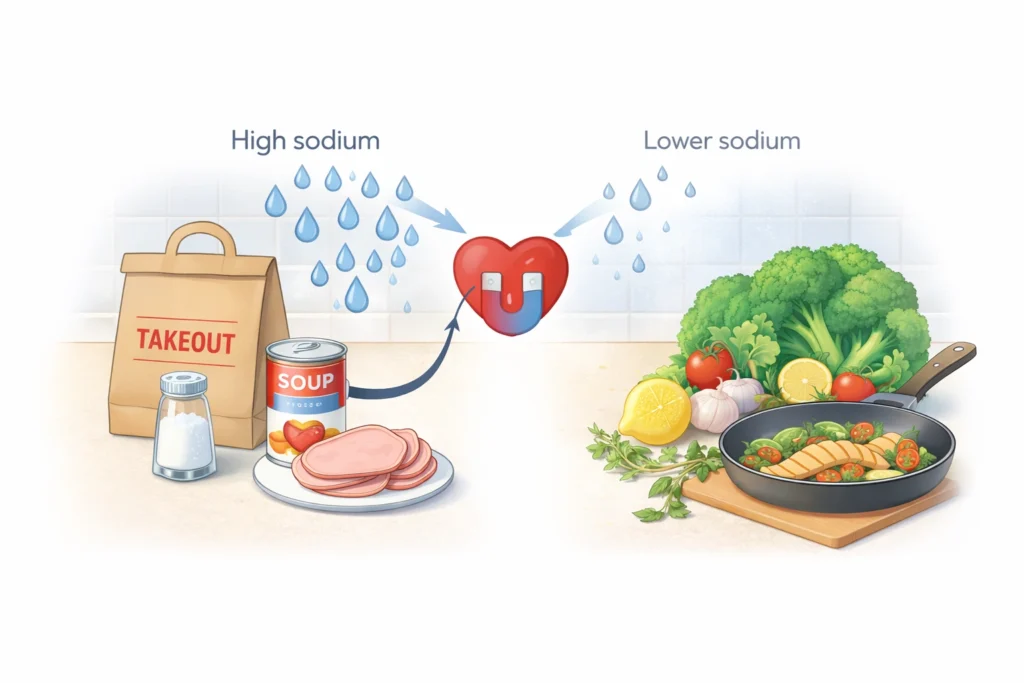
Sodium is the main mineral in table salt. In heart failure, sodium acts like a magnet for water. More sodium in your bloodstream means more water pulled into the blood vessels. The weaker heart has to push against more volume and higher pressure, which usually triggers more shortness of breath, swollen ankles, or sudden weight jump on the scale.
Current research supports a sodium intake below 2,000 milligrams per day for many people with symptomatic CHF, although some providers may go slightly higher or lower based on your condition. For context, 2,000 mg is less than one teaspoon of table salt total in 24 hours. The challange is that most of this sodium is not coming from the salt shaker at home. It hides inside packaged foods like canned soups, frozen dinners, breads, deli meats, marinades, and fast food.
Practical ways to lower sodium without hating your food
We rarely see people succeed by just “trying to use less salt.” Instead, success comes from changing where salt enters the diet in the first place. Some practical steps:
- Choose fresh or frozen vegetables with no added sauces, not canned varieties packed in brine.
- Pick “low sodium” or “no salt added” versions of canned beans, tomatoes, and broths.
- Limit deli meats, bacon, sausage, hot dogs, and cured meats, they are usually extremely salty.
- Cook more often at home so you control what is added to the pan.
- Season with garlic, onion, citrus, black pepper, paprika, herbs, and vinegar instead of salt based blends.
Based on data from recent surveys in the United States, about 70 to 75 percent of daily sodium intake comes from restaurant and processed foods, not from salting at the table. That means small swaps in what we buy and where we eat can have a major impact on heart failure symtoms.
Managing fluids: how much water is too much
Not everyone with CHF needs a strict fluid limit, but many do. When the heart is very weak or when you are having frequent fluid overload episodes, doctors may advise a fluid restriction, commonly around 1.5 to 2 liters per day. This includes all liquids: water, coffee, tea, milk, juices, soups, smoothies, even ice cream when it melts.
A few strategies people often find helpful:
We suggest using a measured water bottle or container so you know your total daily fluid by the time you go to bed. Many of my readers like to fill a 1.5 liter pitcher in the morning and then pour all their beverages from that, so they see how much is left. Spacing drinks across the day, rather than drinking large amounts at once, can also reduce feelings of breathlessness.
If your mouth feels dry because of medication, sucking on ice chips, sugar free hard candy, or even chilled slices of cucumber can help. Remember that high sodium foods will make you more thirsty, so low sodium and fluid control usually work hand in hand.
Building a balanced plate for heart failure

When we talk about a heart healthy diet for congestive heart failure, it helps to picture what a typical plate might look like. We aim for a balance that supports both heart function and overall nutrition:
1. Vegetables and fruits as the base
Fill about half of your plate with non starchy vegetables and, when appropriate, fresh or frozen fruits. These foods bring fiber, potassium, magnesium, and antioxidant compounds that support blood pressure, reduce inflammation, and help control weight.
Good options include leafy greens, carrots, bell peppers, broccoli, zucchini, green beans, berries, apples, pears, and citrus. For those watching potassium due to kidney issues, your healthcare team may tailor which fruits and veggies fit best. It is also smart to limit canned fruit in heavy syrup or salty pickled vegetables.
2. Lean proteins for strength and repair
Muscle loss can sneak up on people with CHF, especially if appetite drops. Protein intake is key for keeping muscles and immune system working. We often aim for roughly 1.0 to 1.2 grams of protein per kilogram of body weight per day for many heart failure patients, with adjustments for kidney function and other health conditions.
Protein sources that usually fit well include:
- Skinless poultry like chicken and turkey baked or grilled
- Fish such as salmon, trout, sardines, and cod, ideally twice per week or more
- Eggs or egg whites
- Low sodium beans and lentils, drained and rinsed to lower sodium further
- Plain Greek yogurt or low fat cottage cheese, if you tolerate dairy
For readers who are curious about more animal based approaches and how they compare with plant forward diets, we go deeper on that debate at this DietLinic article on animal vs plant based diets. Heart failure diets still generally favor plenty of plants, even when animal protein is included.
3. Whole grains for steady energy
Carbohydrates are not the enemy, but refined white breads, pastries, and sugary cereals usually do more harm than good. Whole grains like oats, brown rice, quinoa, barley, and whole wheat pasta give slow burning energy, fiber for digestion, and help support a more stable blood sugar and cholesterol profile.
A sample day might include oatmeal at breakfast, a small serving of brown rice at lunch, and a side of barley or whole grain couscous at dinner. Portion sizes matter if you are also trying to manage weight or diabetes.
4. Healthy fats for heart protection
Healthy fats do not overload the heart; they can actually protect it. Unsaturated fats found in olive oil, avocado, nuts, seeds, and fatty fish have been linked with lower rates of cardiovascular events. We keep portion sizes moderate because fats are calorie dense, but we do not need to fear them.
Mediterranean style patterns rich in extra virgin olive oil and nuts have shown, in multiple studies, reduced risk of major heart events and better long term outcomes. For someone with CHF, swapping butter and shortening for olive or canola oil is a relatively simple but powerful step.
Foods that most people with CHF should limit or avoid
Certain foods tend to hit hard on sodium, saturated fat, or simply calorie overload. Here are the usual culprits that often worsen swelling and shortness of breath within a few days:
- Fast food burgers, fries, fried chicken, and pizza slices
- Canned soups, instant noodles, boxed rice mixes, and flavored pasta packets
- Deli meats, bacon, ham, sausage, and jerky
- Frozen dinners, especially those not labeled “low sodium”
- Snack chips, cheese puffs, salted nuts, and crackers
- Pickles, soy sauce, and bottled salad dressings
A simple “rule of thumb” that many of our readers use is this: if it comes in a crinkly package, a can, or from a drive through window, it probably has more sodium than your heart needs. Checking labels becomes a powerful tool. For a single meal or snack, aiming for less than 500 to 600 mg sodium is a common target, but your doctor may give a custom number.
Alcohol, caffeine, and sweets: how they fit in
Alcohol can interact with heart medication, raise blood pressure, cause heart rhythm problems, and contribute to cardiomyopathy in some people. Many heart failure specialists now lean toward advising little or no alcohol, particularly if alcohol played any roll in the development of heart disease. If your cardiologist allows moderate intake, that usually means no more than 1 small drink per day for women and perhaps up to 1 to 2 for men, though often less is better.
Caffeine from coffee and tea is more nuanced. Light to moderate coffee intake in recent research does not seem to increase heart failure risk and may even be neutral or slightly helpful for some people. But some individuals are very sensitive and feel palpitations or anxiety. Sugary coffee drinks (loaded with cream and syrups) are another story and usually work against both weight and blood sugar goals. Most heart failure patients do well with 1 to 3 cups of plain coffee or tea per day if they tolerate it and if their doctor agrees.
Sugary foods raise triglycerides, contribute to weight gain, and worsen insulin resistance. Desserts do not have to disappear fully, but they should shrink in portion and frequency. Fresh fruit, a small square of dark chocolate, or Greek yogurt with cinnamon often satisfy sweet cravings with less downside.
Sample 1 day meal plan for congestive heart failure
Below is an example of what a heart healthy diet for congestive heart failure might look like across one day. Sodium levels here are rough estimates and depend on exact brands and portions.
| Meal | Menu example | Approximate sodium |
|---|---|---|
| Breakfast | Oatmeal cooked with water, topped with blueberries and a spoon of ground flaxseed; 1 boiled egg; black coffee or tea | ~250 mg |
| Snack | Unsalted almonds (small handful) and an apple | ~5 mg |
| Lunch | Grilled chicken breast (no skin) with mixed green salad, cherry tomatoes, cucumbers, olive oil + vinegar dressing, side of quinoa | ~350 mg |
| Snack | Plain Greek yogurt with sliced strawberries and cinnamon | ~60 mg |
| Dinner | Baked salmon with lemon and herbs, steamed broccoli, small baked sweet potato with olive oil | ~400 mg |
| Daily total | Varies with seasoning and brands | ~1,000 to 1,200 mg |
Someone with a 2,000 mg sodium target would still have room for a pinch of salt in cooking or a small store bought item. The pattern is what matters most: mostly whole foods, cooked simply, with sauces and packaged items limited.
Weight management and heart failure
Weight loss is not always the goal for heart failure. This can suprise people. Some patients enter heart failure after years of obesity and metabolic problems, so dropping extra pounds slowly can help. But others are already normal weight or underweight, especially older adults with advanced disease. Sudden weight loss can mean muscle wasting and worse outcomes.
For those who do need to lose weight, a heart healthy diet focused on volume from vegetables and lean protein, along with smart portions of whole grains and fats, tends to work better than trendy crash diets. Very low carb or very high fat patterns may clash with other conditions and also can be hard to maintain while dealing with fatigue.
On DietLinic we also discuss targeted eating styles like an animal based diet for weight loss. While these can help some individuals, heart failure patients usually need a more cautious, medically guided approach, because fluid balance, kidney health, and medication interactions add extra complexity.
Reading nutrition labels with a “heart failure eye”
Learning to scan labels quickly can change grocery shopping. Over time it becomes almost automatic. For heart failure, three parts of the label really stand out:
- Sodium per serving: Look for under 140 mg per serving when possible. “Low sodium” has a legal meaning in the US and usually fits better than “reduced sodium,” which can still be high.
- Serving size: Many products list unrealistically small portions. If you eat double, remember to double the sodium number too.
- Saturated fat and trans fat: Aim to keep saturated fat low and avoid any product listing “partially hydrogenated oils,” which points to trans fats.
Labels also show added sugars, which can matter for those with diabetes or prediabetes, and fiber content, which is helpful for digestion and heart protection. When in doubt, shorter ingredient lists with words we recognize usually point toward less processed options.
How diet works with medications for heart failure
Most people with CHF are on a group of medicines: diuretics (water pills), ACE inhibitors or ARBs, beta blockers, sometimes SGLT2 inhibitors, mineralocorticoid receptor blockers, and others. Food choices can strongly effect how well these drugs work.
For example, if someone on a diuretic like furosemide eats a very salty meal, the body will hold on to more water, and the pill may not keep up. They may gain 2 or 3 pounds of water weight overnight and feel breathless by morning. On the flip side, if sodium intake is steady and modest, diuretics usually work smoother and with fewer emergency swings.
Certain high potassium foods, like large servings of bananas or orange juice, may need to be restricted when taking medications that raise potassium levels, such as spironolactone or some ACE inhibitors, especially if kidneys are not working perfectly. This does not mean potassium is bad, just that the balance must be monitored with blood tests and medical guidence.
Meal prep tips when you feel tired or short of breath
Fatigue and breathlessness can make cooking feel like a chore. On days when energy dips, we still want you to have access to heart friendly meals. Some practical strategies many heart failure patients use successfully:
- Batch cook simple proteins like chicken breast, turkey, or beans on weekends and freeze in small containers.
- Keep pre washed salad greens, baby carrots, and frozen vegetables on hand. These cut prep time and cook quickly.
- Use a slow cooker or pressure cooker to make low sodium soups and stews that stretch across several meals.
- Ask family or friends to help with grocery runs or chopping vegetables when you are having a tougher week.
Based on what we have seen, people do better when they treat meal prep like a health appointment, not an optional task. Even 30 to 45 minutes once or twice per week can fill the fridge with options that keep you out of the drive through lane.
Monitoring symptoms with daily weight and food choices
Daily morning weight checks are a simple but powerful tool for CHF. Step on the scale after using the bathroom and before breakfast, wearing the same type of clothing. Write the weight down. A sudden gain of 2 to 3 pounds in one day or 4 to 5 pounds in a week often signals fluid build up, even before swelling shows up.
When patients track weight next to a food journal, patterns pop out. A weekend with restaurant meals and salty snacks often lines up with a quick jump on the scale and more shortness of breath. Low sodium, home cooked weeks tend to show more stable numbers and less swelling.
Sharing this log with your cardiologist or dietitian lets them adjust diuretic doses and meal plans in a more targeted way. Many clinics now encourage patients to use simple smartphone apps or even paper notebooks; the key is to make it a daily habit.
Emotional side of changing your diet
Living with congestive heart failure brings fear, grief, and frustration. Food is deeply tied to emotion and culture, so changing the way you eat can feel like one more loss on top of the diagnosis. We see this most around holidays, family gatherings, and comfort foods from childhood.
Allow yourself to feel those reactions. They are valid. It helps to reframe diet changes as an active way you are caring for your heart, not as punishment for past choices. Many families find new traditions, like grilling salmon instead of steaks, or bringing a colorful salad instead of a salty casserole. When loved ones understand that salty foods can literally make it harder for you to breath, most become more supportive.
If you feel overwhelmed, a session with a registered dietitian who works in cardiology can make a huge difference. They can personalize sodium limits, help you read labels, and give recipe ideas that line up with your tastes and cultural background.
Key takeaways for a heart healthy diet in congestive heart failure
A heart healthy diet for congestive heart failure is not about perfection. It is about stacking enough helpful choices so your heart gets a break and your daily symptoms get lighter. Most people do best when they focus on:
- Keeping sodium low, usually below 2,000 mg per day, by limiting processed and restaurant foods
- Working with any fluid limits from your provider and spreading drinks across the day
- Building plates around vegetables, fruits, lean proteins, whole grains, and plant based fats
- Watching daily weight and linking sudden changes with recent meals
- Planning ahead with simple meal prep so you are not at the mercy of fast food when energy dips
Over time, many people notice they can walk farther, sleep better, and have fewer ER visits when they follow a consistent heart healthy eating pattern. This is not just about living longer, but living with more comfort and control. Each lower sodium meal, each home cooked dish, is a small act of kindness toward your heart, and those small acts add up in a very real way.









Leave a Reply